For decades, when people talked about the causes of throat cancer, one factor dominated the conversation: smoking. It made sense. Tobacco exposure had a clear, well-documented link to cancers of the mouth, throat, and lungs. However, something has quietly shifted over the past two decades. In countries like the United States and the United Kingdom, a different risk factor has been rising at a surprising pace. It’s not related to air pollution or diet. Instead, it’s tied to a common and often overlooked aspect of modern relationships, oral sex and its link to human papillomavirus, or HPV.
That headline might sound dramatic at first glance, but behind it is a growing body of research that doctors, oncologists, and public health experts are taking seriously. The real story isn’t about fear or stigma. It’s about understanding how behaviors, viruses, and long-term health risks intersect in ways many people never expected.
So, what’s actually happening here, and how concerned should people be?
A Change No One Saw Coming
Not long ago, smoking was the dominant cause of most throat cancers. Heavy tobacco use damages cells in the mouth and throat over time, creating the perfect conditions for cancer to develop. Public health campaigns, higher cigarette taxes, and changing social norms have all helped reduce smoking rates significantly in many parts of the world. As a result, smoking-related throat cancers have started to decline.
At the same time, though, doctors began noticing something unusual. A different type of throat cancer, specifically oropharyngeal cancer, started increasing. This form affects the tonsils, base of the tongue, and the back of the throat. Unlike traditional cases linked to smoking or alcohol, many of these patients had no history of heavy tobacco use.
That raised an important question. If smoking was declining, what was driving this new wave? The answer led researchers to HPV.
Oral sex has overtaken smoking as the primary driver of throat cancer.
In a significant shift in oncology, the human papillomavirus (HPV) has replaced tobacco and alcohol as the leading cause of oropharyngeal cancer. This specific strain, most commonly HPV-16, targets the… pic.twitter.com/jLi6PaB0a6
— Smart Science (@SmartScience) March 16, 2026
Human papillomavirus is one of the most common viruses in the world. Most people who are sexually active will encounter it at some point in their lives, often without even knowing it. In many cases, the immune system clears the infection naturally within a couple of years.
However, not all HPV strains are harmless. Certain high-risk types, especially HPV-16, can persist in the body. Over time, these infections can trigger cellular changes that may eventually lead to cancer. HPV has long been associated with cervical cancer, but its role in throat cancer is a more recent discovery.
What makes this particularly complex is that HPV-related throat cancer can develop decades after the initial infection. That delay makes it difficult for people to connect the dots between cause and outcome.
How Oral Transmission Plays a Role
HPV spreads through skin-to-skin contact, including sexual activity. That includes oral sex, which can transmit the virus to the throat. Once there, the virus may remain dormant or be cleared by the immune system.
In some cases, though, it lingers. Over time, persistent infection in the oropharyngeal region can lead to abnormal cell growth. Years later, this can develop into cancer. It’s important to stress that this outcome is still relatively rare compared to the number of people exposed to HPV. Most infections never lead to serious health issues. Still, the rising trend is enough to shift how experts think about prevention and awareness.
One of the most striking aspects is how unevenly it affects men and women. Men are significantly more likely to develop HPV-related throat cancer. In fact, some estimates suggest men are three to five times more at risk.
Researchers are still working to fully understand why. Several theories exist. Men may have higher rates of oral HPV infection, possibly due to differences in immune response. Behavioral patterns, such as the number of partners over time, could also play a role. Another factor may be biological differences in how the virus interacts with tissue in the throat. Whatever the reason, the data is clear. This isn’t a gender-neutral trend.
The Numbers Behind the Headlines
In the United States, HPV is now responsible for the majority of oropharyngeal cancer cases. That marks a major shift from previous decades, when tobacco use dominated. In the United Kingdom, similar patterns are emerging, with HPV-related cases increasing rapidly year over year.
Globally, the picture varies. In regions where smoking rates remain high, tobacco still plays a major role. However, in countries where smoking has declined, HPV is becoming the leading driver. This doesn’t mean smoking is no longer dangerous. It still contributes to many cancers and health conditions. Instead, it highlights how multiple causes of throat cancer can evolve depending on behavior and environment.
The rise of HPV-related throat cancer didn’t happen overnight. It developed slowly over decades. One reason is the long latency period between infection and cancer development. A person might contract HPV in their twenties and not develop symptoms until their forties or fifties. By then, the connection is far from obvious.
Another factor is awareness. For years, HPV was primarily discussed in relation to cervical cancer. Public messaging rarely mentions its connection to throat cancer, especially in men. As research advanced, that gap began to close. Doctors started testing tumors for HPV markers, and patterns became clearer. What once looked like a random increase in cancer cases turned out to have a common underlying cause.
Risk Doesn’t Mean Certainty
It’s easy to read headlines like this and assume the risk is immediate or inevitable. That’s not the case. Most people exposed to HPV never develop cancer. The immune system successfully clears the virus in the majority of cases. Even among those with persistent infection, only a small percentage will go on to develop oropharyngeal cancer.
Risk depends on multiple factors, including:
- Duration of infection
- Immune system strength
- Lifestyle habits
- Genetic predisposition
So while oral transmission plays a role, it’s just one piece of a much larger puzzle.
It’s one thing to understand the science behind HPV-related throat cancer, but it often feels more real when you look at how it actually shows up in everyday life. Many cases don’t follow the pattern people expect. There’s no long history of smoking, no obvious high-risk lifestyle, and often no warning that anything serious is developing.
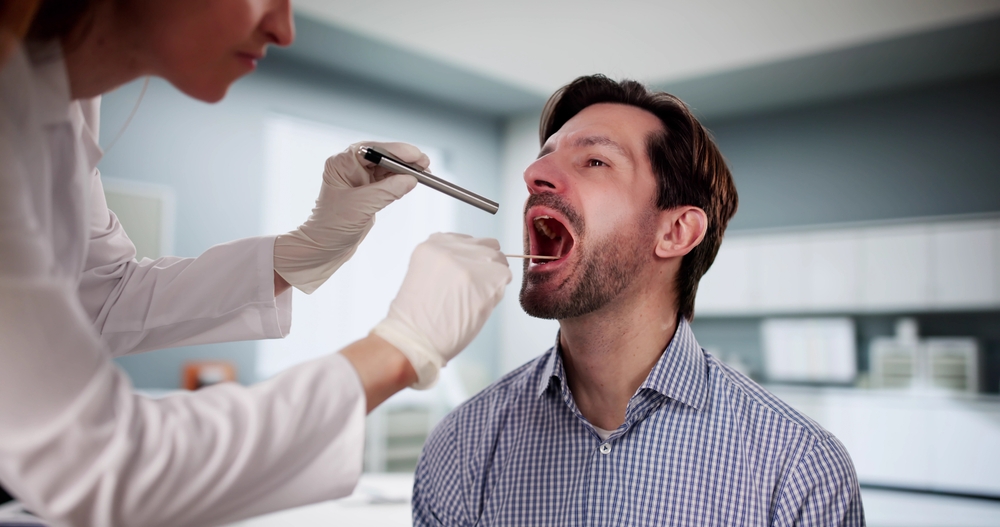
Take a fairly typical scenario. Someone in their forties or fifties notices a sore throat that just doesn’t go away. At first, it feels minor, maybe irritation from a cold or seasonal allergies. Weeks pass, and it lingers. Then there’s a small lump in the neck or a strange discomfort when swallowing. It’s easy to ignore at first, especially when everything else feels normal. Eventually, they go to a doctor.
From there, things tend to move quickly. A general practitioner might refer them to an ear, nose, and throat specialist, often called an ENT. The specialist may perform a scope to look deeper into the throat, followed by imaging scans or a biopsy if something looks unusual. That’s when the unexpected diagnosis can come, oropharyngeal cancer, and in many cases, it tests positive for HPV.
For many patients, that moment is confusing. A common reaction is disbelief. They may think, “I don’t smoke, I don’t drink heavily, how did this happen?” That gap between expectation and reality is one of the reasons awareness still lags behind the data.
Treatment depends on the stage and location of the cancer, but it often involves radiation therapy, sometimes combined with chemotherapy. In certain cases, surgery may also be required. These treatments can be effective, especially for HPV-related cancers, but they aren’t easy. Patients may experience fatigue, difficulty swallowing, changes in taste, or long-term throat sensitivity.
Even so, there is an important point that often gets overlooked. HPV-related throat cancers tend to respond better to treatment than those caused by smoking. Survival rates are generally higher, particularly when the cancer is caught early. That doesn’t make the diagnosis any less serious, but it does offer a level of optimism that’s worth highlighting.
Beyond the physical side, there’s also an emotional layer. People often struggle to understand how they developed a condition linked to a virus they may never have known they carried. There can be hesitation to talk about it openly, partly because of how HPV is transmitted. That can make the experience feel isolating, even though the condition itself is becoming more common.
Stories like this are becoming more frequent, and they highlight why awareness matters. Recognizing symptoms early and understanding the role of HPV can make a meaningful difference. Just as importantly, these real-life experiences help shift the conversation away from confusion and toward prevention, which is where the next part of this discussion becomes especially important.
The Role of Vaccination in Changing the Future
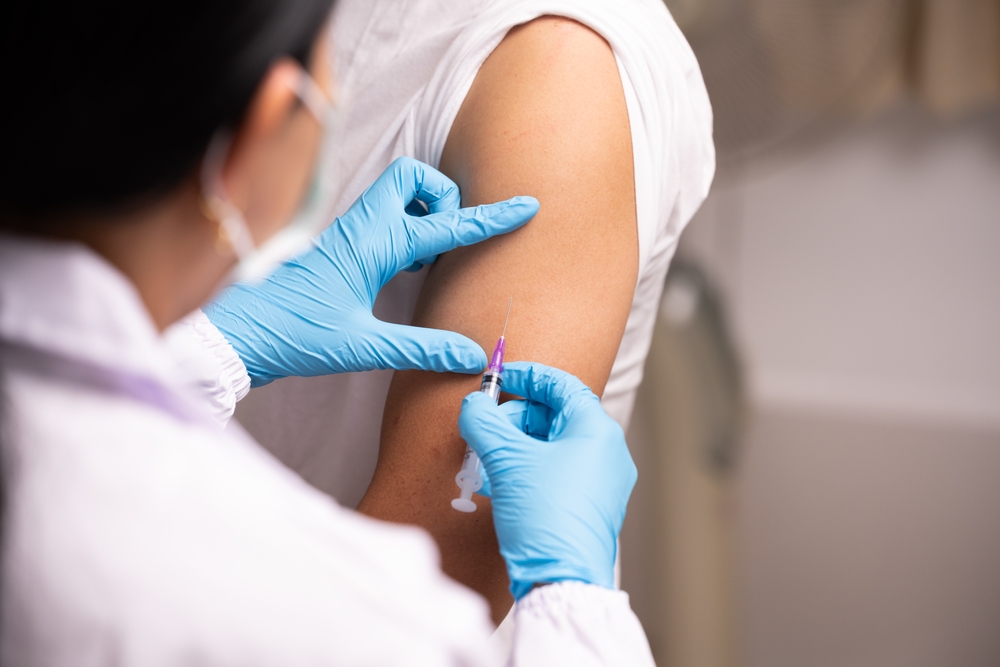
One of the most powerful tools in reducing HPV-related cancers already exists: the HPV vaccine. Vaccines like Gardasil target the high-risk strains of HPV most commonly linked to cancer. Initially promoted to prevent cervical cancer in women, vaccination programs have expanded to include boys as well.
By vaccinating both sexes, public health efforts aim to reduce overall transmission rates. Over time, this could lead to a significant drop in HPV-related throat cancers. However, because of the long delay between infection and cancer development, those benefits may take years, even decades, to fully appear in statistics.
Early Signs People Shouldn’t Ignore
One of the challenges with throat cancer is that early symptoms can be subtle. They often resemble minor infections or everyday discomfort.
Some warning signs include:
- A persistent sore throat
- Difficulty swallowing
- A lump in the neck
- Ear pain without infection
- Changes in voice
These symptoms don’t automatically mean cancer, but they shouldn’t be ignored if they last more than a couple of weeks. Early detection significantly improves treatment outcomes.
The Bigger Picture Around Modern Health Risks
This change from smoking to HPV highlights something broader about modern health. As one major risk declines, another can rise in its place.
It’s not that society has become more dangerous. Instead, behaviors, awareness, and medical knowledge are evolving. What we understand about disease today is far more detailed than it was even twenty years ago. That also means prevention strategies need to evolve.
For example, anti-smoking campaigns remain important, but they’re no longer enough on their own. Public health messaging now needs to include education about HPV, vaccination, and regular health checkups.
Read More: New Study Finds Google AI Can Match or Surpass Radiologists in Detecting Breast Cancer
Moving Beyond the Headlines and Where Research is Heading
Oral sex itself isn’t the direct cause of cancer. The underlying issue is HPV infection, which can be transmitted through various forms of contact. Framing it correctly helps reduce stigma and encourages informed decision-making rather than fear. Understanding that distinction makes a big difference in how people respond to the information.
Scientists continue to study HPV-related cancers to better understand:
- Why do some infections persist while others clear
- How immune responses differ between individuals
- The long-term impact of vaccination programs
- New screening and early detection methods
There’s also growing interest in developing targeted therapies for HPV-related cancers. These treatments could improve survival rates and reduce side effects compared to traditional approaches.
Awareness Without Panic
The idea that a common, everyday behavior could be linked to cancer is understandably unsettling. However, context matters. HPV is widespread, but serious outcomes remain relatively rare. The rise in HPV-related throat cancer reflects changes in behavior, improved detection, and longer life spans, not an immediate crisis.
A balanced approach works best. Stay informed, consider vaccination, and pay attention to persistent symptoms. Those simple steps go a long way in reducing risk.
The conversation around oral sex and throat cancer is evolving. Smoking may no longer dominate the narrative in some countries, but awareness, prevention, and early action remain just as important as ever.
Disclaimer: This information is not intended to be a substitute for professional medical advice, diagnosis or treatment and is for information only. Always seek the advice of your physician or another qualified health provider with any questions about your medical condition and/or current medication. Do not disregard professional medical advice or delay seeking advice or treatment because of something you have read here.
A.I. Disclaimer: This article was created with AI assistance and edited by a human for accuracy and clarity.
Read More: Toilet Paper May be a Source of Cancer-Linked PFAS. 6 Brands to Avoid
