Most of us think of cars as a huge purchase. A reliable new vehicle can cost anywhere from $25,000 to $32,000. But what if a single dose of medicine costs even more than that?
That’s exactly the reality with some modern prescription medications. These aren’t everyday treatments you’d pick up at a pharmacy. Instead, they are highly specialized therapies designed to treat rare, often life-threatening conditions. In many cases, they represent cutting-edge science, from gene therapy to advanced biologics. So why do some treatments cost more than a luxury car, or even a home? And more importantly, who actually pays for them?
1. Hemgenix
If there’s one medication that perfectly captures the idea of “jaw-dropping,” it’s Hemgenix. With a price tag of around $3.5 million, it’s currently one of the most expensive treatments ever approved.
Hemgenix is designed to treat hemophilia B, a rare genetic disorder that prevents blood from clotting properly. People with this condition can experience spontaneous bleeding episodes, which can become life-threatening if not managed carefully. Traditionally, patients need frequent injections of clotting factor throughout their lives.
What makes Hemgenix different is that it’s a gene therapy. Instead of treating symptoms, it aims to correct the underlying genetic issue. It delivers a functional copy of the gene responsible for producing clotting factor IX. In simple terms, it helps the body start doing something it couldn’t do before.
However, that level of innovation comes at a cost. Developing gene therapies involves years of research, complex manufacturing, and strict regulatory approval processes. On top of that, the number of patients who need the drug is relatively small, which means the cost gets distributed across fewer people.
Supporters argue that Hemgenix could replace a lifetime of treatment. When you consider the long-term costs of regular injections, hospital visits, and complications, the price begins to make more sense from a healthcare system perspective. Still, for individuals and insurers, the upfront cost remains staggering.
2. Zolgensma
Zolgensma costs around $2.1 million for a single dose. It’s used to treat spinal muscular atrophy (SMA), a genetic condition that affects muscle strength and movement. In severe cases, infants with SMA may not survive past early childhood without intervention.
What sets this drug apart is its timing. It’s most effective when given early in life, sometimes within the first few months. That means families often face urgent decisions shortly after diagnosis, adding emotional pressure to an already overwhelming situation.
Like Hemgenix, Zolgensma is a gene therapy. It introduces a functional copy of the missing or faulty gene responsible for motor neuron survival. Once administered, it has the potential to significantly improve muscle function and extend life expectancy.
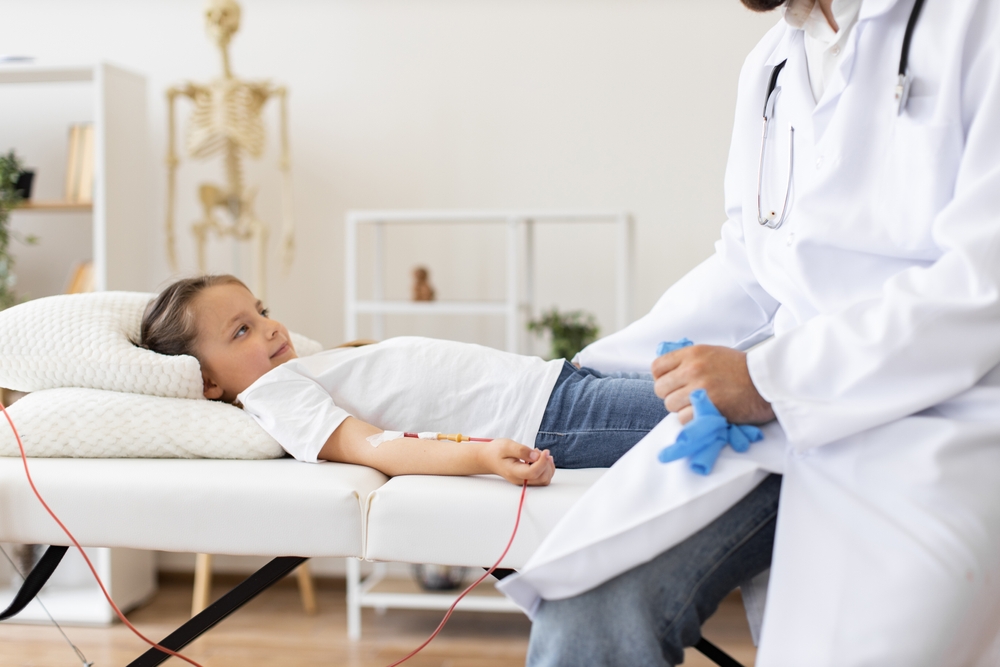
The pricing model here reflects a change in how prescription medications are being developed and sold. Instead of ongoing treatments, companies are creating one-time therapies that aim to provide long-term benefits. While that reduces lifetime medical costs in theory, it concentrates the expense into a single, massive payment.
3. Elevidys
Another recent addition to the world of high-cost therapies is Elevidys, priced at approximately $3.2 million. Duchenne muscular dystrophy (DMD) is a severe genetic disorder that leads to progressive muscle degeneration. It primarily affects boys and often results in loss of mobility and serious health complications over time.
Elevidys represents a new approach. It uses gene therapy to deliver a shortened version of the dystrophin gene, which helps stabilize muscle cells. While it’s not a cure, it has shown promise in slowing disease progression and improving quality of life.
What makes Elevidys particularly interesting is that it highlights how quickly this field is evolving. Just a decade ago, treatments like this were still in experimental stages. Now, they’re becoming part of real-world medical care, although at a very high cost.
For families, the decision isn’t just financial. It’s deeply emotional. When faced with a progressive condition like DMD, the possibility of slowing its effects can feel priceless. Yet, the reality of accessing such expensive prescriptions often depends on insurance approval, location, and healthcare systems.
4. Luxturna
Vision is something many people take for granted, until it starts to fade. For individuals with inherited retinal diseases, that loss can be gradual but devastating. That’s where Luxturna comes in. It costs around $850,000 for both eyes. While it’s lower than some of the other drugs on this list, it still far exceeds the price of most new cars.
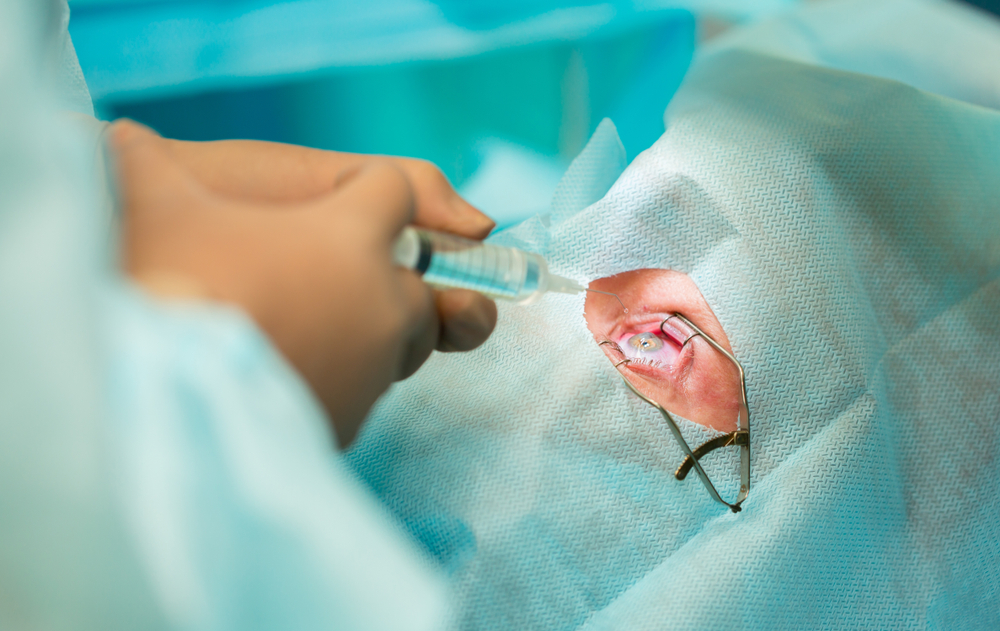
Image credit: Shutterstock.
This therapy targets a specific genetic mutation that leads to vision loss. By delivering a functional gene directly to retinal cells, it can improve vision in patients who would otherwise face progressive blindness. The procedure itself is highly specialized and requires surgical precision and the equipment needed to administer it safely.
Patients taking Luxturna who once struggled to see in low light may regain functional vision. That kind of outcome is hard to measure in purely financial terms. Still, the price raises important questions about access. Treatments like this may exist, but not everyone who needs them can get them.
5. Zynteglo
Zynteglo is priced at roughly $2.8 million and helps treat Beta-thalassemia, a genetic blood disorder that reduces the body’s ability to produce hemoglobin. As a result, patients often require frequent blood transfusions throughout their lives. These transfusions are not only time-consuming but can also lead to complications like iron overload, which requires additional treatment.
Zynteglo takes a different approach. It modifies a patient’s own stem cells to produce functional hemoglobin. Once reintroduced into the body, these cells can reduce or even eliminate the need for regular transfusions. From a scientific perspective, this is a major breakthrough. However, the process is complex. It involves harvesting stem cells, modifying them in a lab, and then reinfusing them after conditioning treatment. Each step requires precision, specialized facilities, and highly trained professionals.
When you look at the lifetime cost of transfusions and ongoing care, Zynteglo can appear more cost-effective in the long run. Still, the upfront price remains one of the biggest barriers. For many patients, access to such advanced prescription medications depends heavily on healthcare systems and funding models.
6. Soliris
Not all expensive medications are one-time treatments. Soliris is a perfect example of how costs can add up over time. Soliris is used to treat rare conditions such as paroxysmal nocturnal hemoglobinuria (PNH) and atypical hemolytic uremic syndrome (aHUS). These disorders can cause severe damage to blood cells, kidneys, and other organs if left untreated.
Unlike gene therapies, Soliris requires ongoing treatment. Patients typically receive regular infusions, often for life. The annual cost can exceed $500,000, which quickly surpasses the price of a new car within just a few months.
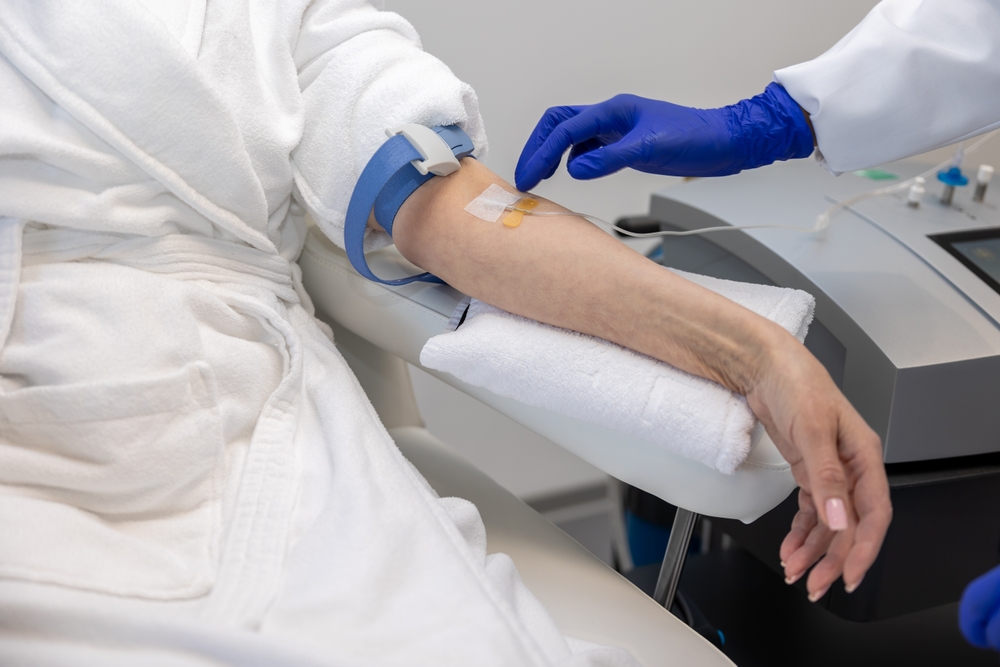
So why is it so expensive? Soliris is a biologic drug, meaning it’s produced using living cells rather than traditional chemical processes. This makes manufacturing more complex and costly. Additionally, like many treatments for rare diseases, the number of patients is relatively small.
Over time, the cumulative cost of Soliris can reach into the millions. Some are expensive upfront, while others become costly due to long-term use. For patients, this creates a different kind of burden. Instead of facing one large decision, they must navigate ongoing treatment, insurance approvals, and potential changes in coverage year after year.
Why Do These Prescription Medications Cost So Much?
The prices of some of these prescription medications can feel almost impossible to justify. However, several clear factors drive these costs, from scientific complexity to how the healthcare system operates. These treatments don’t come off standard production lines. Instead, they require highly specialized processes where precision matters at every step.
One major cost driver is the science behind these therapies. Many go beyond symptom management and aim to fix problems at a biological or genetic level. Researchers must develop advanced technologies, test them thoroughly, and meet strict safety standards. Even small improvements in effectiveness can take years of focused work, and that effort directly shapes the final price.
Manufacturing also adds to the expense. Companies can’t produce these treatments in large, simple batches like traditional medications. Instead, they rely on controlled environments, specialized equipment, and skilled teams. In some cases, they even tailor parts of the treatment to each patient, which makes large-scale production far more difficult. As a result, each dose requires more time, resources, and oversight.

The timeline to bring a treatment to market also plays a role. Teams spend years moving through research, clinical trials, and regulatory approval. Each stage demands funding, coordination, and compliance with strict rules. Even when some projects fail, companies still carry those costs forward into successful treatments.
Market dynamics further influence pricing. When a company develops a unique therapy with little or no competition, it gains more control over how it prices that treatment. While this can encourage innovation, it also raises ongoing concerns about affordability and access.
Who Actually Pays for These Treatments?
While the price tags are eye-catching, most patients don’t pay the full amount out of pocket. Instead, the cost is usually shared across different systems.
In countries with private healthcare systems, insurance companies often cover a large portion of the cost. However, approval is not always guaranteed. Patients may need to meet strict criteria or go through lengthy review processes.
In some regions, government-funded healthcare systems negotiate prices or provide coverage for certain treatments. This can make expensive prescription medications more accessible, but availability may still vary depending on budgets and policies.
In cases where coverage is limited, families may face significant out-of-pocket expenses. This has led to the rise of crowdfunding campaigns and charitable support efforts, especially for rare pediatric conditions.
The Ethical Debate Around Pricing
The existence of these high-cost treatments has sparked ongoing debate. On one hand, these medications represent incredible progress. They offer hope where none existed before. For some patients, they can dramatically improve the quality of life or even extend survival. But on the other hand, the pricing raises serious concerns. Should access to life-saving treatment depend on financial resources or geographic location?
Supporters of current pricing models argue that innovation must be funded. Without financial incentives, companies may be less willing to invest in risky research. Critics, however, point out that healthcare is not like other industries. When the stakes involve human lives, the balance between profit and access becomes far more complicated.
In wealthier countries, patients may have access to advanced treatments through insurance or national healthcare systems. In lower- and middle-income regions, including parts of Africa, access can be far more limited. This creates a gap where the technology exists, but the ability to access it does not
Read More: Largest Study Yet Suggests Medical Cannabis May Help Combat Cancer

Image credit: Shutterstock.
What This Means for the Future of Medicine
Despite the challenges, there’s no denying that medicine is entering a new era.
We’re moving toward:
- Personalized treatments
- Gene-based therapies
- Potential one-time cures for chronic conditions
At the same time, the question of affordability remains unresolved. Will prices eventually decrease as technology becomes more common? Or will the gap between innovation and access continue to grow?
Some experts believe new payment models could help. For example:
- Pay-over-time systems
- Outcome-based pricing
- Government negotiations at a global level
These ideas are still evolving, but they highlight the need for change as medical science continues to advance.
When Innovation Meets Reality
The medications we’ve explored in this article represent years of research, scientific breakthroughs, and, for many patients, a chance at a better life. At the same time, their costs remind us that progress often comes with difficult questions. Innovation can move quickly, but systems that ensure fair access tend to move much more slowly.
So, while these prescription medications may cost more than a brand-new car, their true value goes far beyond money. They sit at the intersection of hope, science, and ethics, forcing us to rethink what healthcare should look like in the future.
Disclaimer: This information is not intended to be a substitute for professional medical advice, diagnosis or treatment and is for information only. Always seek the advice of your physician or another qualified health provider with any questions about your medical condition and/or current medication. Do not disregard professional medical advice or delay seeking advice or treatment because of something you have read here.
A.I. Disclaimer: This article was created with AI assistance and edited by a human for accuracy and clarity.
Read More: 8 Foods That Don’t Mix With Prescription Drugs
